Thousands of autopsies are performed every year in Australia. Who has one and what can they reveal?
Save articles for later
Add articles to your saved list and come back to them any time.
No one saw Tyson Manders fall. One minute, the 26-year-old father of two was off riding motorbikes with his wife’s nephews at their farm. The next, he was lying motionless on the ground. The family had been celebrating a birthday outdoors, laughing over lunch. Tyson’s wife, Georgie, was still sitting at the table when her nephew ran up to find help. The moment she found Tyson, she knew he had died. “I just had this feeling,” Georgie says. “He was still and looked peaceful.”
Time slowed for Georgie as her father and sister tried to resuscitate Tyson. Paramedics confirmed her worst fears – the husband she adored was gone. Tyson and her nephews had been riding safely. Still, as incomprehensible as it was, coming off the bike and landing awkwardly seemed the most likely explanation for what had happened. His body was taken to Sydney for examination.
Tyson Manders, right, in blue cap, beside wife Georgie on the day he died while riding a motorbike on a Yetholme farm.
Days later, Georgie received a call to say there were no signs of any injuries to suggest a bike accident caused Tyson’s death. Would she allow an autopsy? “At first I was firmly thinking no. I didn’t want Tyson’s body being tampered with, I just wanted him home,” Georgie says. “But I kept coming back around to being haunted with the question, ‘Why Tyson?’ There has to be a reason behind this. None of it made sense.”
Whether people we love or know might one day need an autopsy is not something we tend to think about. Most deaths, after all, don’t require investigators to get to the bottom of them. Yet for some deaths, this is a legal requirement. In 2022, 190,775 people died in Australia; of these, forensic pathologists examined about 15,000 bodies.
What happens in an autopsy? Who needs one? And how can investigating a death help the living?
Warning: This article might be disturbing for some readers.
Georgie: “There has to be a reason behind this.”Credit: Wolter Peeters
What’s an autopsy?
At a state mortuary, a technician gently wipes fluid from the mouth of a deceased man. Forensic pathologist Noel Woodford peers at the face, speaking into a dictaphone to record notes for his report. The body is here because the man died unexpectedly. The coroner has authorised the autopsy after considering both the medical grounds for it and any family objections (in this case, there were none). “It’s an unexplained death,” says Woodford, who leads the Victorian Institute of Forensic Medicine (VIFM).
An autopsy, from the Greek “to see for oneself”, can enable pathologists to answer critical questions: How did this person die? What happened in the body that led to death? And – sometimes – what were the circumstances? It can involve inspecting injuries above the skin; opening the body to look at a particular area; or, in full autopsies, examining all organs in the chest, abdominal cavity and sometimes the brain. Despite the TV trope of the forensic pathologist puzzling over murders, most of their work in real life involves natural deaths.
The man’s body faces upwards under bright theatre lights. The skin is pale but the back and the undersides of the arms and legs are crimson because of a process called lividity, where blood pools at the lowest point after circulation stops. Woodford looks closely at the neck, torso and limbs, noting into his dictaphone there are no injuries. He examines the skin for any signs of disease or scarring.
‘If we can do our bit, which is providing answers … we feel like we’ve done a good job.’
The technician makes an incision with a scalpel on each side of the chest – without a heartbeat, there’s no pressure to push blood from the body – then cuts a single line down to the waist, forming a Y. He pulls back the skin, exposing a layer of fat and muscle, then uses clippers to remove a section of the rib cage. Most of the organs are now exposed; the bowel comes out first. “By taking [the bowel] off, we get a better look at the structures on the abdominal wall inside,” Woodford says.
When families ask what happens in an autopsy, Jodie Leditschke, who is the coronial admissions and enquiries manager, describes it as a surgical procedure. “But then we often say to them, ‘What do you want to know?’ because some families want to know exactly what’s happened,” she says. “We have often described to families exactly where the incisions are.” One technique, named after 19th-century Austrian physician Karl Rokitansky, involves removing all organs, from the tongue down to the rectum, as an intact block.
This is done deftly and with great care. “We are always making sure we don’t hurt the deceased, even though we know, in theory, that’s not possible,” Leditschke says. The organs are inspected for clues that can be found in their relationship to one another – the path of an infection, for example, might be visible from one organ to another.
This block of tissue – the workings inside all of us – might be confronting to the untrained eye. To Woodford, it can reveal what he can’t see on a scan: the full extent of old and new plaque in arteries, or the grainy texture of kidneys scarred by high blood pressure. An autopsy, to him, is “a stepwise, regimented approach to looking at tissues”. His observations can help the person’s family. “If we can do our bit, which is providing answers – not just to the coroner or the police, but to them – we feel like we’ve done a good job.”
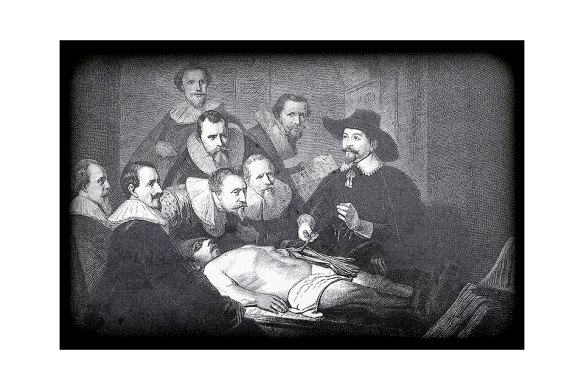
An engraving of Rembrandt’s The Anatomy Lesson of Dr Nicolaes Tulp, from Amsterdam in 1632.Credit: Getty Images
Who needs an autopsy?
One of the first recorded forensic postmortems was on Julius Caesar after his assassination in Rome in 44BC. The physician Antistius concluded that of the emperor’s 23 stab wounds, one to the breast had been fatal, although exactly who delivered it remained unknown. In the Middle Ages, the Catholics set aside their squeamishness to allow plague victims to be autopsied, as well as the body of one of their own, Pope Alexander V, whose successor was suspected of poisoning him (no proof was found). In cultures where prompt burials are customary, such as Jewish and Muslim communities, autopsies were forbidden until later centuries. By the Renaissance, dissections were a regular part of European medical education; the Amsterdam Guild of Surgeons held a public one annually. Their 1632 event, featuring the body of a man hanged for stealing a winter coat, is immortalised in Rembrandt’s The Anatomy Lesson of Dr Nicolaes Tulp.
Today, a death is reported to a coroner in Australia when, generally speaking, it’s unexpected, unnatural or violent. A report also follows someone dying as an unplanned outcome of a medical procedure or while in custody or state care. The coroner then has a legal obligation to take custody of the body to confirm the identity of the person and ascertain what caused their death and, if possible, the circumstances. “We are effectively taking the body into our care so investigations can be made to provide answers to those questions,” says Victoria’s State Coroner, John Cain.
Most natural deaths don’t require investigation if a doctor is satisfied they can record a cause. Queen Elizabeth II’s death certificate, for example, simply stated “old age”. The reason for examining a natural death is often that the person’s medical history can’t explain how they died, says Linda Iles, who heads forensic pathology services at VIFM. “Others may have known chronic disease, but a GP may be unwilling, for a number of reasons, to issue a death certificate,” she says. Accidental deaths, including falls and vehicle or workplace incidents, are also common cases in the mortuary.
Every weekday, a coroner meets with pathologists and staff overseeing admissions and enquiries to “triage” cases. All suspicious deaths receive an autopsy. For others, a CT scan, a toxicology report, an external examination and information from police and doctors might be sufficient to determine the cause of death. Victoria’s mortuary is due next year to be the first in Australia to have an MRI scanner, which will give clearer resolution of brain and heart conditions to complement a CT scan.
These non-invasive examinations have reduced the rate of autopsies. In the early 2000s, for example, nearly every case that arrived at Victoria’s mortuary would receive an autopsy, but now it’s between 35 and 45 per cent – roughly 3000 a year. Initial tests and scans can also rule out causes of death. A Queensland man died after removing a snake from a friend’s leg in September, but preliminary findings were reported to have shown no venom in his system. The family said in a statement an unknown medical condition was now the investigators’ focus.
When any non-suspicious case does require an autopsy, the coroner takes into account the wishes of the dead person’s loved ones before ordering the procedure. “There are those that are very anxious to know what was the ultimate cause of death. And then there’s those that say, ‘Look, the person’s deceased, we’re very sad about it; we just want to get on with the funeral and don’t need to know the precise details’,” Cain says. “Unless there’s some other strong reason to have an autopsy, then we’ll respect the family’s views – and it’s generally around religious or cultural views.” Customs to ensure burials soon after death are still among common objections.
Noel Woodford: An autopsy is a “stepwise, regimented approach to looking at tissues”.Credit: Eddie Jim
Does an autopsy always provide an answer?
In the mortuary, Woodford systematically weighs each organ – the more unusually heavy, the greater the possibility of disease – and examines each for signs of disease, including cancer. He makes tiny incisions a centimetre apart on the heart to check the coronary arteries for a clot or blockage. As he examines each organ, he takes a nick of tissue to examine later under a microscope. Samples of blood and urine will also inform further toxicology tests. The technician photographs organs to ensure another pathologist can review the case if the family or authorities request it.
The procedure takes just over an hour. (A suspicious death takes longer as it involves wider examination and more photography.) Then the technician places cotton wool in the chest and neck cavity. He replaces the chest plate and starts to sew the skin back together. Woodford and the technician return the organs to the body. “It’s important for us to ensure the body is returned to a whole state as much as we can,” Leditschke says. “If we retain organs, we contact the families to let them know.”
Afterwards, just a thin line of neat stitches is visible. “A family, even though they are aware an autopsy has taken place, they actually shouldn’t be able to tell, if he was wearing a singlet or an open-[collared] shirt,” Leditschke says. The technician washes the body with running water, lifting each arm carefully, dries the skin with towels then places a shroud over it and wheels it from the room. It will likely now be released, with a provisional cause of death if the coroner allows. In Victoria, the body is generally in the mortuary for between four and seven days before the coroner releases it to a funeral home.
‘It can open up other lines of inquiry that go to the circumstances in which somebody died.’
The body of Woodford’s own father came to the mortuary after he died suddenly of a stroke. It was the 1990s, and Woodford, who had been a trainee at the institute, was working elsewhere. He felt what the process was like from the outside as a family member. “I was really amazed at how respectful everybody was, and sympathetic.” He also appreciated how important it was to get a death certificate to manage finances. In cases where a coroner is yet to establish a cause of death, the registry can issue an interim death certificate, although this might not be accepted for all financial purposes.
Pathologists do often find a single underlying cause such as a clot in an artery. More puzzling cases can involve a confluence – death certificates typically ask for a hierarchy of events but can allow for several causes to equally contribute. “As we get older, we have more things going on,” Iles says. “Or, in younger people, say, you’ve got one disease process going on but you’ve got some drug use going on as well; or you find yourself in a physical circumstance that is adverse. It can become quite complex.”
If an autopsy, microscopy, scans and toxicology results aren’t able to provide a conclusive answer, the cases can be referred to further specialists. Genetic testing can consider heart rhythm disorders that can’t be seen under a microscope such as Long QT syndrome, Brugada syndrome or the tachycardia known as CPVT. In about 5 per cent of cases, Woodford says, the cause of death remains “unascertained”, although an autopsy can at least exclude possibilities such as trauma or infection.
Once an autopsy report is complete, it allows the coroner to either finalise the case or consider it as part of a wider investigation. “It can open up other lines of inquiry that go to the circumstances in which somebody died,” Cain says. The coroner can hold an inquest where a court hears evidence, or make written findings that are published based on public interest. In other cases, the autopsy report becomes part of a criminal investigation and prosecution.
Johan Duflou: “Every so often we come up with something which is of major concern.” Credit: Brook Mitchell
Are autopsies ever like in the crime shows?
Sydney forensic pathologist Johan Duflou felt his “spidey senses tingling” while autopsying the body of an elderly woman in 1989. The woman had injuries to the back of the head that didn’t appear like a typical fall. The police attended the autopsy – a wallet had been missing – and Duflou recalls one theory being the death could be a “mugging gone wrong”.
But the pattern of the injuries bothered him. He told police he suspected it was a homicide. The woman turned out to be a victim of Sydney’s so-called “granny killer”, John Wayne Glover, who in 1990 was convicted of murdering six women. Glover hit several of his victims with a hammer. “Obviously, we’re not police officers,” Duflou says. “But we investigate deaths. Every so often we come up with something which is of major concern.”
Crime-show portrayals of forensic analysts as world-weary oddballs don’t sit well among real-life practitioners. “It is not only misconceived, it makes us very much annoyed to see us portrayed that way,” Duflou says. “We’re all different. Some of us have more foibles than others.” Says Iles: “When you look at the forensic pathologists we have on staff here, our youngest are young women. We don’t have any of the crusty old-professor type at all.”
‘It’s whether the injuries make sense in the context it’s been put to you.’
As on TV, pathologists do occasionally attend police scenes, but only if there’s a medical or investigative question they can help address, such as uncertainty surrounding a death being suspicious. Cain will be notified of deaths such as a police shooting, or someone dying in custody, so he can attend the scene if he chooses. “You just get a much better idea of what’s happened,” he says.
In real-life suspected homicides, the autopsy will be fast-tracked, with pathologists and police working together closely: without context from police and the scene, whether someone has been assaulted, had an accident or inflicted a wound themselves can be difficult to distinguish. “It’s whether the injuries make sense in the context it’s been put to you,” Iles says. The devil can be in the detail. If someone has injuries on a single plane of their face, they might have fallen, whereas a fight or self-defence can leave scattered injuries. “It’s not always the actual fatal wound itself but potentially smaller injuries that give you information,” says Iles.
The autopsy will also consider whether the person’s health played a role. “It’s not exactly rocket science that they’ve been shot or stabbed, but it’s the [surrounding information] that the autopsy is for – not just for the prosecution but for the defence.” Depending on the case, the hands, fingernails or injuries can carry trace evidence that helps police identify suspects or objects of interest. Pathologists take swabs but are rarely privy to the results. “We’re not necessarily about who did it,” Iles says.
Linda Iles: “I have a job to do and it’s to solve problems.”Credit: Eddie Jim
How do the experts deal with seeing death up close?
It can be a challenging field, but those interviewed for this article say their work isn’t different from the emergency or medical workers who confront the same scenes. “When it comes to seeing confronting, and, you know, potentially quite gruesome things, I have a job to do and it’s to solve problems,” Iles says. Roger Byard, an emeritus professor at the University of Adelaide, puts it this way: “The way that pathologists survive is because we treat it as a scientific exercise.”
The cases can affect these professionals, though. The most tragic for Byard was that of a young woman who he discovered had been buried alive. Her ex-boyfriend subsequently pleaded guilty and was sentenced in August. Byard received a forensic science award for his work on the case, but the horrible finding lingers. “I did come up with the right diagnosis. And yes, he did plead guilty. But it’s a case that I find very difficult to find anything positive about.”
Leditschke’s first day as a technician at the mortuary in 1988 went smoothly – “I was so excited” – but the next day she passed out. “It was sights, sounds, realising that I’m standing there among so many deceased persons.” Quiet cases are the ones that have particularly affected her and her colleagues: when lonely people die without family, or youngsters have died at similar ages to children in their own lives. In some of the hardest cases, the technicians have made plaster casts of the feet of infants for the families. “That’s just something the mortuary staff took up.”
After decades of working with technicians, and now also managing a team who speak to grieving families, Leditschke sees the job from both sides: “To ensure you respect the body … you can’t completely [say] this is just an anatomy,” she says. “What you’re dealing with is a recent death where, right at that time, there is a family grieving.“
Byard has done more than 6000 autopsies, and he is proud of research that found a gene involved in sudden infant death syndrome. But even with all his experience, kissing the forehead of his father after he died still shocked him. “He was so cold and waxy. Death can be confronting even to somebody who deals with it every day,” he says. “I was looking at him in the funeral home, thinking, it has to be him. But he looked different. Death is a difficult process.”
Georgie with Aaron and Elaina in their memorial garden for Tyson. Credit: Wolter Peeters
How can understanding death help the living?
On the farm where Tyson Manders died, a garden grows with a sign that says “daddy’s spot”. This is where Georgie and their two children go to remember him. Georgie’s family has kept bees in Yetholme, near Bathurst, for four generations, and at the centre of the memorial is a bee box. The family leaves letters and mementoes such as carved pumpkins on Halloween. “He was a very hard-working, fun-loving, seemingly healthy, strong young man,” Georgie says.
The autopsy revealed it wasn’t a bike accident that caused Tyson’s death, but a heart condition called hypertrophic cardiomyopathy. Counsellors told Georgie it was probably instant. “I found a lot of peace of mind knowing that,” she says. “We all held a lot of guilt thinking at first that it was a bike accident. We were doing CPR, we were doing everything we could; did we overlook something? There was nothing we could have done … He wouldn’t have experienced any pain.”
Often a deceased person’s loved ones will ask mortuary workers whether they could have done anything to save the person. “More often than not there isn’t,” says Natalie Morgan, a family liaison nurse at VIFM. “We always tell the truth, but you do try to emphasise reassurance wherever possible.” Sometimes loved ones want to know why the body appeared a certain way; if they saw the body with blood coming from the nose or mouth they might believe the person was injured. Morgan explains this is often due to a sudden fluid build-up after the heart stops. “It can just be part of the normal process of dying.”
Another common question is what the time of death was. Iles says crime shows have perpetuated the myth that pathologists can accurately determine this. “Occasionally, people have pacemakers and bits and pieces and we can interrogate those,” she says. “Circumstantial information is often a lot more reliable than the rate of decomposition.”
In some cases, an autopsy flags an opportunity for genetic screening for family members, including for cancers, neurological conditions and heart disease. Around one in 500 people carry a genetic variation that could lead to a heart condition, says Chris Semsarian, a cardiologist and geneticist at the Royal Prince Alfred Hospital. “You can save lives by doing good, comprehensive autopsies,” he says. Georgie now knows Tyson carried a gene that has a 50 per cent chance of being passed down to their children, Elaina, 10, and Aaron, 7. Tyson’s autopsy has brought back a sense of control for Georgie: “I think knowledge is power.”
The children now receive regular heart checks and are preparing to do the testing. If they carry the gene, medication can help manage the condition. “Tyson has left behind a legacy,” Georgie says. “My husband’s life and the father of our children will protect our future generations just with that knowledge of the cause behind his death.”
Get fascinating insights and explanations on the world’s most perplexing topics. Sign up for our weekly Explainer newsletter.
If you'd like some expert background on an issue or a news event, drop us a line at [email protected] or [email protected]. Read more explainers here.
Most Viewed in National
Source: Read Full Article